Iron
I. Storage form = ferritin (Iron + protein)
II. Functions
A. Iron (heme) + protein (globulin) = hemoglobin
1. Oxygen transport
B. Myoglobin, muscle protein
C. Enzyme activation (co-factor)
III.
Deficiency
A. Iron deficiency anemia
1.
Fewer (#) red blood cells
2.
Less hemoglobin
3.
Pale mucus membranes
B. Reduced appetite (pica)
C. Diarrhea
D. Labored breathing
E. Rough hair coat
F. Decreased growth
Newborn animals susceptible (pigs)
IV. Toxicity
A. Free Fe are very toxic
B. Fe always associated with a protein
C. 2 Fe + 1 ß globulin protein (transferrin) = transferritin for Fe transfer
Selenium
I. Functions
A. Component of glutathione peroxidase
1. Protect against oxidation of PUFA
B. Protect tissue from toxic substances
C. Interrelationship with Vit. E
1. Spare each other
II. Deficiency
A. White muscle disease (stiff lamb disease)
B. See Vit. E
III. Toxicity
A. Blind staggers or Alkali disease
1. Emaciation
2. Loss of hair
3. Soreness and sloughing of hooves
4. Blindness
5. Death
|
Mineral |
Main Functions |
Deficiency
Symptoms |
Comments |
|
Calcium (Ca) |
Bone and teeth formation; blood
coagulation; muscle contraction; nerve function; cell permeability;
milk production; egg shell formation |
Rickets (young); osteomalacia
(adult); tetany; thin-shelled eggs; reduced egg production; hypocalcemia or milk fever in dairy cattle |
Vitamin D involved in absorption and bone deposition; excess PO4 decreases absorption; excess Mg decreases absorption, replaces Ca in bone and increases Ca excretion; Ca:P ratio should be 1:1 to 2:1 |
|
Phosphorus (P) |
Bone and teeth formation;
phosphorylation; high-energy phosphate bonds; PO4 chief
anion radical of intracellular fluid; PO4 important in acid-base
balance |
Rickets (young); osteomalacia
(adult); reduced egg production |
Vitamin D involved in renal reabsorption and bone deposition; excess Ca and Mg causes decrease in absorption; Ca:P ratio should be 1:1 to 2:1; in male ruminants, excess P may cause urinary calculi |
|
Soduim (Na) |
Major cation of extracellular
fluid where it is involved in osmotic pressure
and acid-base equilibrium; preservation of normal muscle cell
irritability; cell permeability |
Reduced growth; eye
disturbances with corneal lesions; reproduction
impairment (infertility in males, delayed sexual maturity in females) |
Salt tocicity readily occurs in nonruminants with levels above 8% in diet; staggering gait, blindness, nervous disorders and hypertension |
|
Chlorine (Cl) |
Major anion involved in osmotic
pressure and acid-base balance (chlorine shift); hydrochloric acid in
digestion |
Hypochloremic alkalosis (usually due to physiological disturbance such as vomiting rather than deficiency); reduced growth |
Toxicity unlikely |
|
Magnesium (Mg) |
Enzyme activator primarily
in glycolytic system; bone formation |
Vasodilation; hyperirritability with convulsions, loss of equilibrium and trembling; tetany |
Excess upsets Ca and P metabolism; toxicity not likely |
|
Mineral |
Main Functions |
Deficiency
Symptoms |
Comments |
|
Potassium (K) |
Major cation of intracellular
fluid where it is involved in osmotic pressure
and acid-base balance; muscle activity |
Hypokalemia; lethargic condition with high incidence of comas and death; diarrhea, distended abdomen and unitidy appearance |
Excess reduces Mg absorption; Mg deficiency reduces K retention leading to K deficiency |
|
Sulfur (S) |
Sulfur-containing amino acids;
SH group function in tissue respiration; component of biotin and thiamine |
Primarily reduced growth effect due to sulfur amino acid requirement for protein synthesis |
Toxicity unlikely |
|
Iron (Fe) |
Cellular respiration (hemoglobin, cytochromes, myoglobin) |
Hypochromic-microcytic anemia
(less than normal amount of hemoglobin and fewer red cells); anemia may be
common in baby pigs unless Fe is supplied |
Ca-P ratio influences absorption; Cu required for proper metabolism; pyridoxine deficiency decreases absorption |
|
Copper (Cu) |
Cofactor in several
oxidation-reduction enzyme systems; hemoglobin synthesis; bone formation;
maintenance of myelin of nerves; hair pigmentation |
Fading hair coat or lack of wool; nervous symptoms or ataxia; lameness, swelling of joints and fragility of bones; anemia |
Excess Mo or Zn inhibit its utilization and storage; toxcity occurs at levels above 250 ppm with much the same symptoms as deficiency |
|
Zinc (Zn) |
Component or cofactor of several enzyme systems including
peptidases and carbonic anhydrase; needed for bone and feather development |
Poor hair or feather development and slipping of wool; rough and thickened skin or parakeratosis in swine |
High Ca or phytate ties up Zn; excess Zn interferes with Cu metabolism and may cause anemia |
|
Mineral |
Main Functions |
Deficiency
Symptoms |
Comments |
|
Manganese (Mn) |
Thought to be an activator of enzyme systems involved in oxidative phyosphorylation, amino acid metabolism, fatty acid synthesis and cholesterol metabolism; bone formation (organic matrix); growth and reproduction |
Poor growth; shortened long bones;
impaired reproduction (testicular degeneration of males, defective
ovulation of females); perosis or slipped tendon in poultry |
Excess Ca and P decreases absorption; toxicity unlikely |
|
Cobalt (Co) |
Component of vitamin B12;
needed by rumen bacteria for growth and vitamin B12 synthesis |
Anemia (varies from
normocytic-normochromic to megaloblastic or macrocytic); deficiency in
ruminants causes reduced appetite, reduced growth and body weight and eventually
death |
Related in vitamin B12; toxicity unlikely |
|
Iodine (I) |
Thyroxine formation |
Goiter; stillbirths;
hairless pigs or wool-less lambs at birth |
Long-term intake of high amounts of I reduces thyroid uptake of I |
|
Selenium (Se) |
Component of the enzyme glutathione peroxidase, which reduces peroxides arising from tissue lipid oxidation; thus, protects against cellular membrane damage by the peroxides; functions are closely related to that of vitamin E |
Excudative diathesis (chicks); muscular dystrophy (white muscle disease); cattle stiff lamb disease-sheep; liver necrosis (pigs, rats) |
Chronic toxcity yields blind staggers at 10-20 ppm or alkali disease at 5-10 ppm; acute toxcity occurs at 20 ppm and above; sudden death; SO4 protector against toxcity |
|
Molybdenum (Mo) |
Purine metabolism;
stimulates microbial activity in rumen |
Lack of conversion of xanthine to uric acid but not likely to be deficient in natural diet |
Excess interferes with Cu activation of enzymes; causes anemia and diarrhea; SO4 protects against toxcity |
|
Fluorine (F) |
Traces protect against teeth decay |
Excesses of F are of more concern than deficiencies in livestock production |
Levels above 5-10 ppm block vital oxidative enzymes by interfering with Mn; causes bone deformities enamel defects and organ degeneration; Ca and Al salts protect against toxcity; F is a cumulative poison so toxicity may not be noted for some time |
INTEGRATION OF METABOLISM
Well Fed State:
Glucose is the source of energy for the brain
AA to liver for protein
Excess AA used for energy - trans- and de-amination ( urea synthesis)
Fats go to adipose tissue
CHO for NADPH production
Starvation:
Nothing coming for the diet
Sources of nutrients:
Fat (stored in adipose tissue)
Glycogen (liver & muscle)
Brain uses glucose, but not muscle
Early starvation, muscle uses ketone (FA, but limited number available)
Can only break down so much protein - only 25-30% of muscle an be broken down.
Brain can be eventually forced to used ketone bodies for energy
Hormones
Insulin: Polypeptide (51 AA) - produced by b cells of Islets of Langerhans in Pancreas. Anabolic (synthesize glycogen, triglycerides, protein)
Regulation: of secretion (what stimulates secretion)
1. High blood glucose (hyperglycemia) after a meal
2. High blood amino acids after a meal
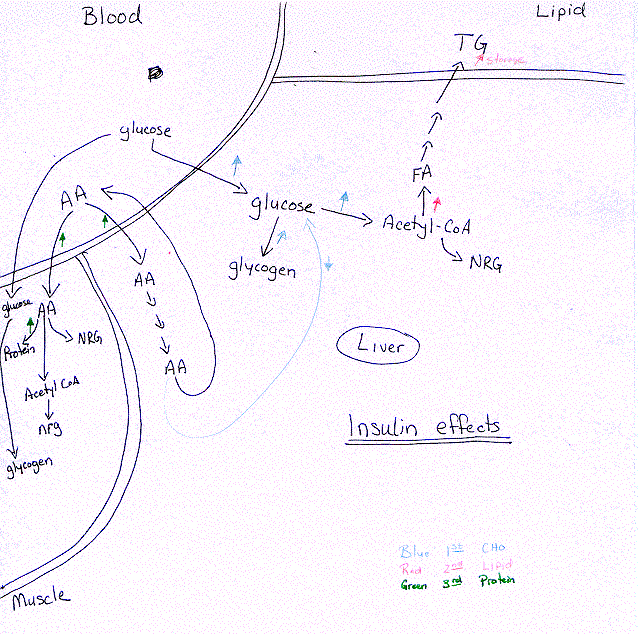
Metabolic effects - due to binding to receptors in liver, muscle, adipose tissue.
1. CHO Metabolism - Prevent hyperglycemia by ¯ blood glucose
a. Increase glucose transport into adipose and muscle cells
b. Increase glycolysis (glucose ® acetyl-CoA)
c. Decrease gluconeogenesis in the liver
d. Increase glycogen synthesis in liver and muscle
2. Lipid Metabolism Promotes lipogensis (triglyceride synthesis in adipose tissue)
a. Increase fatty acid synthesis: 1) Acetyl-CoA from glucose (glycolysis); 2) NADPH from glucose
b. Increase triglyceride synthesis
c. Increase triglyceride storage in adipose tissue
3. Amino Acid Metabolism Reduce blood AA increasing synthesis
a. Increase entry of AA to liver and muscle cells
b. Increase protein synthesis
c. Increase degradation of surplus AA
d. Urea cycle activity
Glucagon: Polypeptide (29 AA) produced by a cells of Islets of Langerhans in Pancreas. Catabolic - favors breakdown of glygogen in liver, mobilization of fatty acids, protein degradation, and gluconeogenesis (oppose the action of insulin)
Regulation: - Low blood glucose (hypoglycemia) after overnight or prolonged fast.
Metabolic Effects - due to binding to receptors in liver & adipose tissue ONLY!!
1. CHO Metabolism - Prevent hypoglycemia by mobilization and synthesis of glucose
a. Increase glycogen breakdown in liver (NOT muscle = no receptors)
b. Increase gluconeogenesis by activating key gluconeogenic enzymes
2. Lipid Metabolism - promotes lipolysis (breakdown)
a. Increase triglyceride breakdown - release free FA
b. Increase mobilization of FA and uptake by the liver
c. Increase b -oxidationin liver - Acetyl-CoA
d. Increase ketone body formation
3. Amino Acid Metabolism - lowers AA concentration in the blood
a. Increase uptake of AA by the liver for gluconeogenesis
b. Other hormones (cortisol) degradation of muscle protein, release AA into blood